
Delhi6:35 PM | 27th April 2024
Despite higher prices in the private sector, people still prefer to go there only because of the absence of doctors and healthcare workers along with quality constraints of the public sector.

In a country as populous as India, ensuring adequate healthcare services for its citizens is a monumental challenge. The doctor-patient ratio, a key indicator of healthcare accessibility, has been a matter of concern in India for years. Education Post’s Prabhav Anand explores the current situation of healthcare sector in India, delving into the doctor-patient ratio, healthcare infrastructure, and the impact of COVID-19 on the healthcare sector.
I was recently on a visit to one of the most prominent hospitals in the capital when saw that Vijay Ram, a 25-year-old boy, musters a weak cough as he was struggling to get up from the hospital’s gate. When I asked them about their situation, they told me something that made me write this article. “We are here for the last three days,” says Manjay Ram, the grandfather of Vijay as the two waited in a line of over 200 patients outside the hospital’s main gate, seeking an appointment.
“No doctor has been able to find out the exact problem of this disease so far. We’ve been to many hospitals around our district but nothing happened,” says Manjay in a deep-throated voice. But finally, one private hospital doctor in the district suggested taking him to this hospital and consulting the doctor here where he can get the right treatment.
Manjay, who comes from a small village in Bihar’s Munger district, more than 1,300 kilometers from New Delhi, doesn’t have any appointments and doesn’t even know any doctor’s name.
His only option is to wait patiently, hoping to secure one of the limited slots available each morning.
This story of people like Manjay plight and countless others who rise at the first light to join the queue is a stark reminder of the big scarcity of specialized doctors and healthcare professionals in rural India, where more than two-thirds of its 1.4 billion population resides.
Now imagine a country where millions of people are in dire need of medical attention, but there aren’t enough doctors to meet their needs. Picture hospitals overflowing with patients, long queues extending down hallways, and precious minutes slipping away as individuals wait desperately for medical care.
India is grappling with the daunting task of providing adequate healthcare services to its vast population. Among the many challenges faced by the Indian healthcare system, the issue of the doctor-patient ratio looms large. With an ever-increasing population and a shortage of healthcare professionals, ensuring accessible and quality healthcare for all remains a significant concern.
The doctor-patient ratio, a critical metric for evaluating the availability and accessibility of healthcare professionals, serves as a crucial indicator of the healthcare system’s capacity to meet the needs of patients. In India, the current doctor-patient ratio stands at approximately 1:834, a figure that is considerably good in comparison to the World Health Organization’s (WHO) recommended ratio of 1:1000. But the question still arises, is this data true? Although this data by NMC (National Medical Commission) has not been officially released anywhere, instead the statement was given by Minister of State for Health and Family Welfare Bharati Pravin Pawar, replying to a question asked by Rajya Sabha member Kanimozhi N.V.N Somu on July 26, 2022.
Inaugurating the first specialized medical institute in northeast India in April, Prime Minister Narendra Modi said that his government had sought to increase the number of doctors by setting up more medical colleges. “This deficiency was a major barrier to quality health services in India,” he said. “Therefore, our government has worked on a large scale to increase medical infrastructure and medical professionals in the last nine years.”
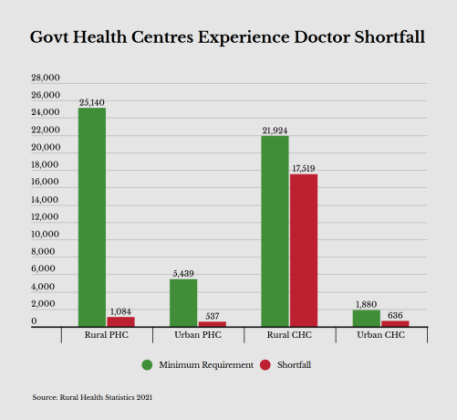
According to the World Health Organisation (WHO), India’s doctor-patient ratio hit a record high of 1.2 doctors per 1,000 patients in 1991, but as its population surged, the ratio dropped to about 0.7 in 2020.
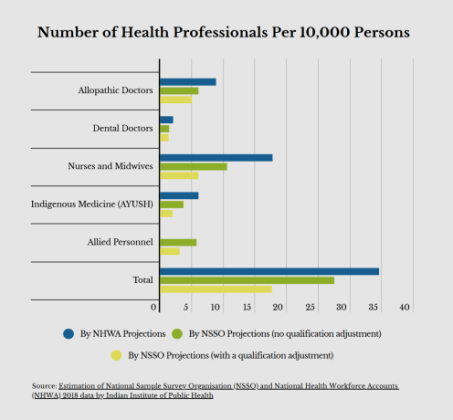
PM Modi’s government has built more than a dozen similar medical institutes for specialized treatment since he took office in 2014. The government has plans to build at least one major hospital in each of India’s 761 districts. But the problem is the lack of doctors, a shortage that is reaching crucial levels as India becomes the world’s most populous nation. The number of public hospitals, excluding specialized institutes, has risen some 9% in Modi’s time at the top, government data shows.
Recently the Modi government has highlighted the opening of 23 AIIMS hospitals and the coverage of 50 crore persons under the Ayushman Bharat scheme. The budget outlays for the establishment of the new AIIMSs has not only seen tardy implementation but massive budget overruns from the original estimate of Rs. 650 crore to close to Rs. 7,000 crore. Most of these institutes are yet to get fully functional.
This money could be well spent on strengthening thousands of CHCs and PHCs that are in their most pitiable state. The poor people should be given the basic health facility first instead of giving them the option to choose AIIMS for their treatment.
The consequences of a high doctor-patient ratio are multifaceted. Overcrowded hospitals and clinics are a common sight nowadays, resulting in longer waiting times and stretched resources. Patients often have limited access to primary care physicians, leading them to seek specialized care in tertiary hospitals, further burdening an already strained system. The lack of adequate medical attention can compromise the quality of care provided, impeding timely diagnosis, treatment, and follow-up care.

“India’s doctor-patient ratio has long been a pressing concern, and addressing it requires a multi-faceted approach. The challenges contributing to the poor ratio are rooted in various factors like Burgeoning Population, Urban-Rural Disparity, Brain drain of doctors, and Limited Medical Education Infrastructure,” says Abhinav Nikunj, a resident doctor at NMCH Sasaram Abhinav added, “To rectify the doctor-patient ratio in India and improve healthcare accessibility, several measures should be considered like scaling up medical education, incentivizing rural services, augmenting healthcare infrastructure, embracing telemedicine and technology, and public-private collaborations.”
In India, the healthcare sector is mostly dominated by private healthcare providers. During the early ’50s, when the share of the private sector was around 8 percent, but now it has grown up to 70 percent. Almost two-thirds of doctors in the country are working in the private sector.
The National Sample Survey Household Social Consumption Statistics 2017-18 revealed that for private healthcare settings, the cost of hospitalization is seven times more than that of government hospitals.
Even then people prefer private hospitals even after their high expenses. Only 30 percent of the overall population prefers going to government hospitals to seek treatment for their illness. Whereas 43 percent of the people prefer going to private doctors or private clinics for their treatment, 23 percent people prefer private hospitals and almost 4 percent people prefer to go to charity-based hospitals.
According to research by Factchecker.in, every four out of 10 people choose a government hospital for their in-patient hospitalization.
Despite higher prices in the private sector, people still prefer to go there only because of the absence of doctors and healthcare workers along with quality constraints of the public sector.
The COVID-19 pandemic had a profound impact on the healthcare sector in India. The surge in cases exposed the underlying weaknesses in the healthcare system, including the shortage of healthcare professionals, inadequate infrastructure, and insufficient funding. Overburdened hospitals, scarcity of critical medical supplies, and overwhelmed healthcare workers were among the challenges faced during the peak of the pandemic.
However, the crisis also led to some positive changes. The Indian government took various measures to strengthen the healthcare system, including increased funding, expansion of healthcare facilities, and efforts to augment the healthcare workforce. Telemedicine emerged as a crucial tool for remote consultation, reducing the burden on physical hospitals and improving accessibility to healthcare services.
Copyright© educationpost.in 2024 All Rights Reserved.
